 Expert's opinion
Expert's opinion
The article is a subjective view on this topic written by writers specializing in medical writing.
It may reflect on a personal journey surrounding struggles with an illness or medical condition, involve product comparisons, diet considerations, or other health-related opinions.
Although the view is entirely that of the writer, it is based on academic experiences and scientific research they have conducted; it is fact-checked by a team of degreed medical experts, and validated by sources attached to the article.
The numbers in parenthesis (1,2,3) will take you to clickable links to related scientific papers.
Colon Broom Reviews 2024: Is It Worth It & Legit?
All articles are produced independently. When you click our links for purchasing products, we earn an affiliate commission. Learn more about how we earn revenue by reading our advertise disclaimer.
8.5
Quality
7.8
Support Research
8.8
Reputation
7.6
Price
Features
- Eliminates toxins in the body
- Ingredients are natural
- Vegan and 100% gluten-free
- Increases metabolism rate
- Aids weight loss
- Promotes rise in energy levels
Brand Information
- Established in 2008
- Based in Fremont, Nebraska
- Producer of natural supplements
Medical Benefits
- Relieves diarrhea
- Improves gut health
- Relieves constipation
- Treats bloating
Colon Broom Discount + Free Shipping: CBOFF10
About ColonBroom
ColonBroom is manufactured by Max Health Nutrition LLC. It was founded in 2008 in Fremont, Nebraska. The company’s chief executive officer is Josh Mcyntire.
Max Health Nutrition LLC specializes in health and supplementary dietary additives. Their products are available on their official online store and on Amazon.
ColonBroom is a colon cleanser made from all-natural ingredients that help improve digestive health and relieve constipation and bowel problems. It also carries additional health and long-term benefits,[1] such as decreased blood sugar, reduced insulin levels, increased metabolic rates, and improved general gut health.
Their company policy requires you to fill in a quick digital questionnaire based on your medical history. This data collection aims to personalize your medical experience and provide customer-tailored medical service. It is free and fast.
What Is ColonBroom?
Colon Broom is a fiber-based supplement that helps alleviate diarrhea and improves general gut health[2]. It helps remove toxins and promotes regular bowel movements. It is vegan and gluten-free. In addition, it is a powerful supplement with thousands of favorable reviews and testimonials.
ColonBroom has additional health benefits, such as aiding in weight loss, increasing metabolic rates, improving metabolic health, and lowering blood sugar.
It is safe for most people with allergic reactions. It is a bulk-forming laxative that absorbs water in the colon, which helps improve gut health, deal with constipation, relieve bloating, and increase probiotic activity in the colon.
Feature Product & Coupon

Colon Broom
- Helps in weight loss
- Improves general gut health
- Aids weight loss
- Information on third-party testing is lacking
- Does not cater to all allergies
- Bloating may happen during the first few days
Colon Broom Discount + Free Shipping: CBOFF10
Does ColonBroom Really Work?
Yes, it does. ColonBroom seeks to resolve gut health by providing an effective dietary supplement. Colon Broom targets the root cause of irregular bowel movement that may help achieve a healthier gut.
It helps alleviate constipation, relieves bowel pains, and improves your general digestive health. The main ingredient, psyllium husk powder, helps boost the immune system.
Consistent usage is recommended for people who struggle with chronic constipation or those who seek to lose weight. When paired with additional weight loss products, ColonBroom achieves better weight loss results.
ColonBroom Ingredients
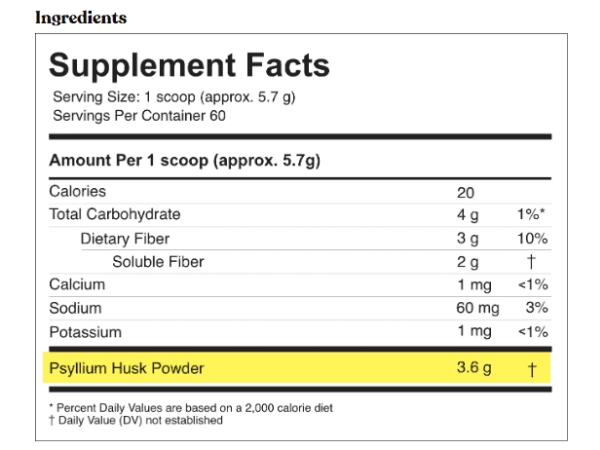

ColonBroom is a safe and easy-to-use supplement. It contains bulk-forming laxatives, dietary fibers, and essential minerals.
It is non-GMO and gluten-free, and all sources are natural. Psyllium Husk Powder, an essential fiber, is its main ingredient.
It has additional ingredients; potassium, sodium, calcium, calories, and carbohydrates such as dietary and soluble fibers.
One container consists of 60 servings per container, with each scoop containing approximately 5.7 grams.
Each scoop of ColonBroom is approximately 5.7 g. It contains 1 mg of potassium, 60 mg of sodium, 1 mg of calcium, 20 mg of various calories, 4 g of carbohydrates, and 3 g of dietary fiber, of which 2 g are soluble fibers.
Psyllium husk is primarily a soluble fiber with a minimal amount of insoluble fiber in it. Other ingredients include citric acid, stevia leaf, crystallized lemon, sea salt, fruit and vegetable juice, rice hulls, and natural flavoring.
Psyllium Husk Powder
Psyllium husk powder helps relieve constipation and aids in weight loss by controlling appetite, with the end result being fewer calories consumed. It also boosts the body’s immune function[3] by promoting a healthy colony of microorganisms in the body’s microbiome.
Citric Acid
Citric acid is a weak organic acid that helps promote nutrient digestion and mineral absorption[4]. Repetitive use of organic acids leads to the thickening of the intestinal walls. It also helps regulate cholesterol levels[5] and triglycerides.
Crystallized Lemon
Crystallized Lemon is a compound that helps reduce fat, prevent the formation of kidney stones,[6] and maintain safe cholesterol levels. It also acts as a stimulant for the digestive system to function better and improves overall gut health.
Stevia Leaf Extract
Stevia leaf extract Is used as a sweetener and an alternative to artificial sweeteners. It has numerous benefits, including lowering blood pressure and blood sugar levels[7]. It is also beneficial in weight loss management as it contains low levels of calories.
Sea Salt
Sea salt provides a wide range of health benefits[8]. It helps keep blood pressure normal. It improves skin health and is advantageous to overall digestive health. It helps cleanse the colon and acts as a laxative. It relieves constipation and helps detoxify the body.
Other ingredients include Silicon dioxide. Silicon Dioxide is a naturally occurring compound consisting of silicon and oxygen.
Colon Broom Reviews From Real Users
With this being said, you might want to check out what real users say about the brand, its excellent customer service, its free shipping, and other company services.
You’ll be glad to know that most of the ColonBroom reviews range from a 3-star review to a 5-star review showing how much effort they give to please their customers.
5 stars
I have had a recurring constipation problem. I’ve tried a few other dietary supplements, and it’s been ineffective until I tried ColonBroom. I love how painless it is to take it. I noticed the difference in a week. I’ve had people tell me that I’ve lost weight around my stomach and back. It makes me feel better. Love the taste.
Laurel C.
4 stars
It’s fine in general, I had a little bloating, but I think that was okay. It also tastes nice. The problem I think, is that it’s slightly overpriced. I feel like there needs to be a fairer price.
Mia D.
Alternatives To ColonBroom

Gundry MD PrebioThrive
See Gundry MD PrebioThrive Review
- Free Shipping
- 90-day money-back guarantee
- Supports bone health
- Expensive pricing
- Prolonged results

Athletic Greens
- Supports immunity
- Improves nervous system
- Certified by the National Sanitation Foundation (NSF)
- May cause gastrointestinal side effects.
- The uncertainty that ingredients are clinically relevant

BioX4
- It is 100% natural
- It is safe
- Improves overall health
- May cause flatulence
- May cause mild bloatedness
Health Benefits Of ColonBroom
Boosts Probiotic Growth
Colon Broom contains several probiotic properties that promote healthy probiotic growth in the gut. Colon Broom also contains citric acid that helps thicken intestinal walls and strengthens the intestinal barrier.
Promotes Weight Loss
Soluble fibers, like psyllium husk powder, are known for lowering fat absorption and helping in weight management. This is because it blocks fats during digestion. In this case, fats don’t get absorbed, making it easier to trim excess fats that may accumulate in areas such as the waistline.
ColonBroom’s powder is made from soluble fiber that helps you lose weight faster. It also improves healthy gut bacteria, creating a better foundation for those who want to start a more nutritious weight-loss regimen.
Improves Overall Digestive Health
Psyllium helps improve the gut microbiota. A 2019 study[9] found that psyllium husk supplementation improved bacteria growth and maintenance.
These bacteria are associated with the production of short-chain fatty acids vital for immune health and maintaining the strength of the intestinal walls.
Improves Mood
Several studies[10] have found that increased levels of fiber are associated with lower depression. This may be due to improvement in gut bacteria, hormone and neurotransmitter production, and inflammation reduction.
The lightness linked to bowel movement may be attributed to the vagus nerve. The vagus nerve is one of the longest nerves in the body, running from the brain to the large intestine.
Bowel movements, especially after constipation, may cause enough stress to the vagus nerve to trigger vasovagal syncope[11], otherwise known as poophoria. If the body has a mild stress reaction to the vagus nerve triggering, it could lower your blood pressure; as a result, you might feel lighter.
However, if your vagus nerve overreacts to the body’s stress of having a bowel movement, it could cause you to faint.
People relieved from constipation may also feel lighter due to a reduction in abdominal distention, i.e., swelling of the stomach, which can cause bloatedness.
Lowers Blood Sugar Levels
Taking fiber supplements helps control the body’s glycemic response[12] to certain meals. The main ingredient of ColonBroom, Psyllium husk powder, carries certain properties that help reduce blood sugar and insulin levels.
This is because the gel-forming fibers in psyllium slow down the digestion of food, which, in turn, helps regulate insulin and blood sugar levels.
Promotes Better Metabolism
ColonBroom encourages improvement in overall health and blood pressure. The product’s main ingredient, Psyllium husk powder, can be beneficial for heart health and blood glucose. Increased intake of psyllium may also help curb high blood pressure[13].
This improvement in blood pressure may effectively reduce the chances of atherosclerosis-related cardiovascular disease risk.
Psyllium can help improve properties linked to metabolic syndrome. This includes cholesterol, blood pressure, and blood sugar level reduction.
Potential Side Effects
ColonBroom has no adverse side effects. However, a number of patients have experienced bloating within the first few days of using ColonBroom. Should this happen, consult a doctor.
Other than bloating, there are no other adverse side effects of ColonBroom. Should negative symptoms appear in use, consult your doctor. It is extremely important to drink enough fluid while taking ColonBroom for it to work properly. A lack of fluid in conjunction with a high fiber intake can cause constipation and potential impaction or acid reflux.
ColonBroom has no side effects for pregnant women and is completely safe for breastfeeding moms and those trying to conceive. However, pregnant women, breastfeeding women, and those trying to conceive should consult a doctor before beginning use.
How To Take ColonBroom
ColonBroom should be taken twice a day. Take one teaspoon of powder with 250 ml of water, along with an extra glass of water to increase colon efficiency. It is advisable for first-time users to take only one serving for the first five days. They can gradually increase the dosage of two servings as per their physicians’ directives.
A gradual increase in fiber gives the body time to adjust and minimizes the chances of adverse side effects such as gas and bloating.
ColonBroom should not be taken immediately before going to bed. It is advisable to take the supplement for at least 30 minutes or an hour before going to sleep.
ColonBroom should never be taken after taking other medications. This is because other drugs may interfere with the ColonBroom medication since it deals with the digestive system. To achieve maximum efficiency, use ColonBroom as advised by your doctor. Those with various allergies should also seek further consultation before using ColonBroom.
ColonBroom Results Before And After: Is It Worth Buying?
ColonBroom has been in the market for some time now. The company boasts of over 100,000 clients so far and has received a lot of backing from customer reviews. A large number of users feel relieved of constipation after regular intake of Colon Broom.
ColonBroom online stores offer a health quiz that generally seeks to understand your health history and produce the most appropriate medicinal schedule tailored for its clients.
ColonBroom has a sweet taste, making it easier to take, and doesn’t leave a bad aftertaste. Symptoms generally seem to ease as patients continue usage for the first 2-3 weeks, with patients experiencing good stool behavior within two weeks of beginning use. Minimal bloating is normal since it is an adjustive reaction by the stomach to Colon Broom.
However, the bloating should subside in a matter of days and therefore be no cause for concern. Constipation should generally ease within four weeks of regular use. ColonBroom not only solves constipation, bloatedness, and irregular bowel movements but also improves overall gut health by improving the growth of good gut bacteria.
Improvement in digestive health contributes to the well-being of the immune system. ColonBroom seems to have zero known side effects, and it leaves you generally feeling lighter.
The formula improves the gut’s efficiency with just one supplementary dietary fiber. Using ColonBroom leaves customers experiencing healthy regular bowel movements.
Final Thought
ColonBroom helps improve general gastrointestinal health. It helps improve gut health, and bowel movement and generally makes you feel lighter and better.
The product ranges from about $27.99 and is recommended to people with food reservations, such as vegans; it is gluten-free and safe for people who are lactose intolerant and people looking to consume natural products.
Thousands of reviews list ColonBroom as a life-changing product. At least one ColonBroom review found the product to be too pricey, so cost is a definite factor.
The quiz, however, appears to be a little abstract. The product is exempt from people with certain allergic conditions. The product appeals to customers with irritable bowel movements, mild constipation, and low fiber intake or who may want to support their weight loss journey.
There is a visible lack of transparency concerning return policies. Dosage also seems to vary from person to person, and one might experience bloating for the first few days. However, it sometimes persists and could signal a need to discontinue the product. If negative symptoms persist, discontinue the usage and seek further medical consultation from a doctor.
Anyone seeking a fiber-based colon cleanser should consult their doctor before initiating use.
Frequently Asked Questions
ColonBroom is a natural, fiber-based dietary supplement. It tastes good and relieves constipation, and bloating, and improves overall gut health.
The ColonBroom quiz is rather vague. It is especially inconclusive for people with certain allergies.
ColonBroom has properties that aid weight loss. Although it works differently among clients, it is a general consensus that ColonBroom users lose weight. Customer reviews have suggested that ColonBroom helps ease the weight loss journey for those using other weight loss supplements. Consult a doctor before use.
ColonBroom relieves constipation, improves overall gut health, and improves digestive health. It is popular and accessible on Amazon and online stores from ColonBroom.
Colon Broom can be purchased from Amazon or the ColonBroom official website.
+ 13 sources
Health Canal avoids using tertiary references. We have strict sourcing guidelines and rely on peer-reviewed studies, academic researches from medical associations and institutions. To ensure the accuracy of articles in Health Canal, you can read more about the editorial process here
- Anderson, J.W., Allgood, L.D., Turner, J., Oeltgen, P.R. and Daggy, B.P. (1999). Effects of psyllium on glucose and serum lipid responses in men with type 2 diabetes and hypercholesterolemia. The American Journal of Clinical Nutrition, [online] 70(4), pp.466–473. Available at: https://pubmed.ncbi.nlm.nih.gov/10500014/
- Weickert, M.O. and Pfeiffer, A.F.H. (2008). Metabolic Effects of Dietary Fiber Consumption and Prevention of Diabetes. The Journal of Nutrition, [online] 138(3), pp.439–442. Available at: https://academic.oup.com/jn/article/138/3/439/4670214
- Agrawal, R. (2021). Psyllium: A Source of Dietary Fiber. [online] ResearchGate. Available at: https://www.researchgate.net/publication/354837462_Psyllium_A_Source_of_Dietary_Fiber.
- Fikry, A.M., Ismail Elsayed Attia, Ismail, I.E. and Reda, F. m (2021). Dietary citric acid enhances growth performance, nutrient digestibility, intestinal microbiota,… [online] ResearchGate. Available at: https://www.researchgate.net/publication/352352857_Dietary_citric_acid_enhances_growth_performance_nutrient_digestibility_intestinal_microbiota_antioxidant_status_and_immunity_of_Japanese_quails
- Khan, Y., Rafeeq Alam Khan, Syeda Afroz and Siddiq, A. (2010). Evaluation of hypolipidemic effect of citrus lemon. [online] ResearchGate. Available at: https://www.researchgate.net/publication/261276322_Evaluation_of_hypolipidemic_effect_of_citrus_lemon
- Gul, Z. and Monga, M. (2014). Medical and Dietary Therapy for Kidney Stone Prevention. Korean Journal of Urology, [online] 55(12), p.775. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4265710/
- Jan, S.A., Habib, N., Shinwari, Z.K., Ali, M. and Ali, N. (2021). The anti-diabetic activities of natural sweetener plant Stevia: an updated review. SN Applied Sciences, [online] 3(4). Available at: https://link.springer.com/article/10.1007/s42452-021-04519-2
- Lee, B.-H., Yang, A.-R., Kim, M.Y., McCurdy, S. and Boisvert, W.A. (2016). Natural sea salt consumption confers protection against hypertension and kidney damage in Dahl salt-sensitive rats. Food & Nutrition Research, [online] 61(1), p.1264713. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5328355/
- Jalanka, J., Major, G., Murray, K., Singh, G., Nowak, A., Kurtz, C., Silos-Santiago, I., Johnston, J., de Vos, W. and Spiller, R. (2019). The Effect of Psyllium Husk on Intestinal Microbiota in Constipated Patients and Healthy Controls. International Journal of Molecular Sciences, [online] 20(2), p.433. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6358997/
- Faezeh Saghafian, Hajishafiee, M., Rouhani, P. and Parvane Saneei (2022). Dietary fiber intake, depression, and anxiety: a systematic review and meta-analysis of epidemiologic studies. [online] ResearchGate. Available at: https://www.researchgate.net/publication/357572364_Dietary_fiber_intake_depression_and_anxiety_a_systematic_review_and_meta-analysis_of_epidemiologic_studies
- Aydin, M.A. (2010). Management and therapy of vasovagal syncope: A review. World Journal of Cardiology, [online] 2(10), p.308. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2998831/
- Brennan, C.S. (2005). Dietary fibre, glycaemic response, and diabetes. Molecular Nutrition & Food Research, [online] 49(6), pp.560–570. Available at: https://pubmed.ncbi.nlm.nih.gov/15926145/
- Clark, C.C.T., Salek, M., Aghabagheri, E. and Jafarnejad, S. (2020). The effect of psyllium supplementation on blood pressure: a systematic review and meta-analysis of randomized controlled trials. The Korean Journal of Internal Medicine, [online] 35(6), pp.1385–1399. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7652639/



