 Expert's opinion
Expert's opinion
Expert's opinion
The article is a subjective view on this topic written by writers specializing in medical writing.
It may reflect on a personal journey surrounding struggles with an illness or medical condition, involve product comparisons, diet considerations, or other health-related opinions.
Although the view is entirely that of the writer, it is based on academic experiences and scientific research they have conducted; it is fact-checked by a team of degreed medical experts, and validated by sources attached to the article.
The numbers in parenthesis (1,2,3) will take you to clickable links to related scientific papers.
Signs Of Dehydration In Pregnancy, Causes & How To Prevent 2024

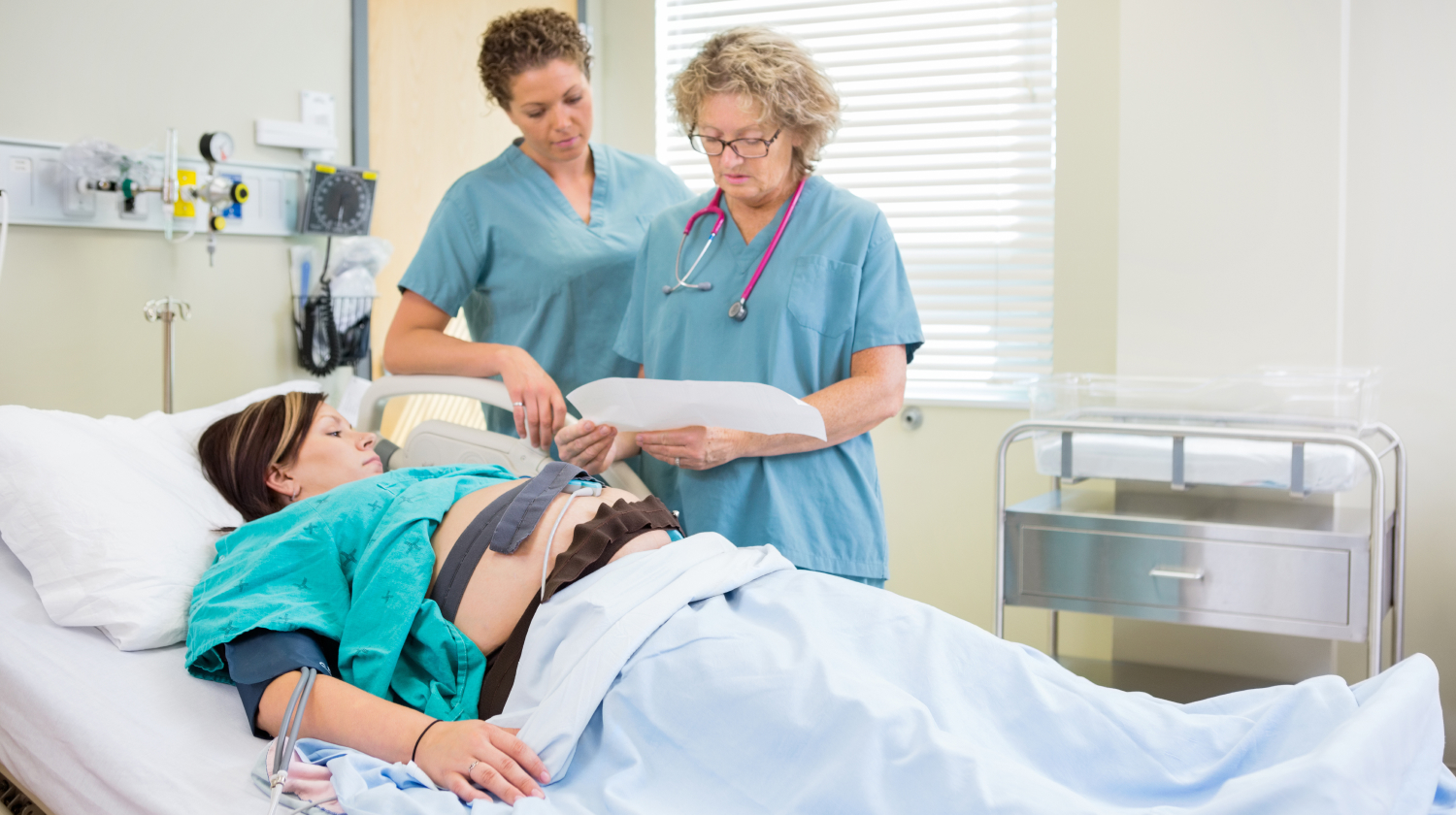
As a pregnant woman; it’s vital to recognize the signs of dehydration during pregnancy to prevent any complications for both you and your baby. Some common signs of pregnancy dehydration include low urine output, fatigue, low blood pressure, severe morning sickness, and low amniotic fluid.
These signs can appear as early as the first trimester and continue. Severe dehydration can lead to serious pregnancy complications, so drinking plenty of fluids throughout the day is essential to avoid dehydration.
Let’s discuss the causes of dehydration during pregnancy, its signs, and practical steps to prevent it. You will understand why adding plain or sparkling water to your everyday diet is prudent.
Signs Of Dehydration During Pregnancy
Some signs of dehydration during pregnancy include:
- Low urine output.
- Dry mouth and throat.
- Fatigue.
- Dizziness.
- Headaches.
- Constipation.
- Reduced fetal movement.
- Maternal overheating.
- Nausea.
Causes Of Dehydration In Pregnancy
The primary cause of dehydration is inadequate water. In pregnancy, the stakes are higher since it’s two lives, not just one.
So here are some causes of dehydration in pregnancy:
Hormonal Changes
Hormonal changes[1] during pregnancy can affect your body’s water balance, causing more fluid loss. Hormones such as progesterone relax blood vessels in the kidneys, leading to more volume filtered and, with that, more excretion. This leads to more water and electrolytes lost in the urine and an increased risk of dehydration.
Exercise
Strenuous exercise may cause excessive sweating, leading to severe water loss and redistribution of electrolytes.[2] As the body temperature rises during exercise, the body sweats to cool itself down, which can result in a significant fluid loss if not replaced adequately.
Severe Morning Sickness
Both common morning sickness, and the more serious hyperemesis gravidarum,[3] can dehydrate. The loss of fluids and electrolytes from vomiting can lead to dehydration.
Dehydration may cause dry mouth, dark urine, and dizziness. The fluid loss may reduce cardiac output, leading to low blood pressure.
Urinary Tract Infections, i.e., UTIs
You become highly susceptible to contracting an upper urinary tract infection or UTI[4] when pregnant. The weight of the uterus can cause partial obstruction of the urinary tract, swelling it — physiologic hydroureter[5] — and any standing fluids in the body can attract bacterial growth. Therefore, it’s crucial to drink plenty of fluids to flush out bacteria
8 Signs Of Dehydration In Pregnancy
Dehydration during pregnancy can have severe consequences for both you and your baby. So here are eight signs of dehydration:
Low Urine Output

If you’re not urinating as frequently as usual, this could indicate dehydration. Low urine production occurs when the body tries to conserve water by reducing the urine produced.
Dry Mouth And Throat

Dehydration causes dry mouth because the body doesn’t have enough fluids to produce saliva. When dehydrated, your body prioritizes retaining water for vital organs, reducing saliva production.
As a result, you may have difficulty speaking or swallowing.
Fatigue

When the body is dehydrated, total blood volume decreases, leading to low blood pressure, and reduced blood flow and oxygen delivery to the muscles and organs. This can make you feel more tired than usual.[6]
Dehydration causes an electrolyte imbalance crucial in regulating muscle and nerve function, causing muscle weakness[7] and fatigue.
Dizziness

When dehydrated, your body doesn’t have enough blood volume to maintain normal blood flow. As a result, your heart rate has to increase to compensate, often unsuccessful, for your blood pressure drop.
Low blood pressure can lead to dizziness[8] or lightheadedness, especially when standing up quickly or exerting yourself. Nausea can follow.
Headaches

The body’s lack of fluids may also trigger headaches or migraines,[9] although the exact way it does is still unclear. While pregnancy may improve migraine headaches, dehydration can negate this effect.
Constipation

Not drinking enough water can cause constipation, especially if you take pregnancy protein powder which might aggravate it. The body strives to retain as much water as it can when it is dehydrated, so it o absorbs water from the colon. This can lead to firmer, more difficult-to-pass stools.
Inadequate hydration can also make it more difficult for stool to pass through the colon.
Reduced Fetal Movement
Your amniotic fluid levels[10] turn over every hour, so it’s a dynamic process dependent on your blood pressure and hydration. A reduction in amniotic fluid gives the fetus less space to move around, leading to a perceived decrease in fetal movement. A severe reduction of fluid and fetal movement suggests a problem with the pregnancy, independent of hydration.
In severe cases, dehydration can cause contractions when premature labor must be ruled out.
Maternal Overheating

Dehydration can cause maternal overheating during pregnancy when your body can no longer regulate its internal temperature. Increased body temperature can complicate your developing pregnancy. Maternal overheating during pregnancy can cause dehydration to worsen as your body sweats more in an attempt to cool down.
Once you have some or most of these signs, it is best to boost your water intake at once and supplement using an oral rehydration solution[11] to replenish the lost fluids.
Complications From Dehydration In Pregnancy
Complications to your pregnancy from dehydration:
Reduced Amniotic Fluid Levels
Dehydration can lead to reduced amniotic fluid levels, which are completely reversible. When it isn’t, it indicates serious problems[12] with the pregnancy itself, not necessarily dehydration.
Neural Tube Defects
Dehydration during early pregnancy is associated with neural tube defects[13] in the baby, such as spina bifida. However, inadequate hydration’s association with these doesn’t mean it causes them. More studies are needed.
Baby Weight and Length
Dehydration may affect[14] the baby’s weight and length. Still, the associations between them encourage staying hydrated throughout pregnancy.
Inadequate Breast Milk Production
Reduced milk production[15] can be a dehydration complication during pregnancy and lactation. Your body may prioritize vital organs, reducing blood flow to non-essential organs such as your breasts.
This can interfere with breast milk production and its composition, leading to lower volume and nutritional value.
Reduced Blood Volume
During pregnancy, total blood volume increases[16] to support the growth and development of your baby. Dehydration can reduce plasma volume, leading to complications such as low blood pressure, dizziness, and fatigue.
Preterm Labor
Preterm labor is a potentially serious complication causing delivery of your baby before 37 weeks of gestation. Dehydration can decrease blood volume and increase drinking only when thirsty, which increases oxytocin production[17] to cause contractions and cervix dilation.
Maternal overheating and lower amniotic fluid levels in the sac from dehydration can also contribute to contractions.
How To Prevent Dehydration During Pregnancy
How much water should a pregnant woman drink?
Experts recommend drinking 3 liters of water daily when pregnant to prevent dehydration during pregnancy. You may also drink coconut water, sparkling, or lemon-flavored water if you cannot stand plain water.
Drinking water and other fluids helps to increase breast milk production and maintain a healthy blood volume and pressure.
To prevent dehydration, you should drink water and other healthy fluids regularly throughout the day and develop healthy dietary habits, including plenty of fruits and fruit juices. Fruits like watermelons and veggies like cucumbers and zucchini could help.
If you are having trouble drinking water during pregnancy, one actionable step is always to carry a water bottle to sip on as you go about your day. Do this as you run errands, rest, and especially when exercising.
Even so, please ensure that the water is safe from contamination which may lead to diarrhea during pregnancy.
The Bottom Line
Staying hydrated during pregnancy is crucial for the expecting mother and her developing baby. Dehydration can lead to preterm contractions and reduced blood volume.
You can catch and rectify dehydration symptoms early, such as urinating less, i.e., volume, not frequency, low-grade fever, nausea, dizziness, and rapid pulse. It is recommended that expecting mothers drink around 8 to 12 glasses of water daily, or approximately 2 to 3 liters daily. This volume may vary depending on individual needs and environmental factors like hot weather.
One way to monitor hydration is to check the color of your urine, aiming for a pale yellow color. By prioritizing drinking water and monitoring your water intake, you can ensure normal bodily functions, establishing a solid foundation for a healthy pregnancy and an unproblematic delivery.
+ 17 sources
Health Canal avoids using tertiary references. We have strict sourcing guidelines and rely on peer-reviewed studies, academic researches from medical associations and institutions. To ensure the accuracy of articles in Health Canal, you can read more about the editorial process here
- Tkachenko, O., Shchekochikhin, D. and W. Schrier, R. (2014). Hormones and Hemodynamics in Pregnancy. International Journal of Endocrinology and Metabolism, [online] 12(2). doi:https://doi.org/10.5812/ijem.14098.
- Maughan, R.J. (1991). Fluid and electrolyte loss and replacement in exercise*. Journal of Sports Sciences, [online] 9(sup1), pp.117–142. doi:https://doi.org/10.1080/02640419108729870.
- London, V., Grube, S., Sherer, D.M. and Abulafia, O. (2017). Hyperemesis Gravidarum: A Review of Recent Literature. Pharmacology, [online] 100(3-4), pp.161–171. doi:https://doi.org/10.1159/000477853.
- Zhang, N., Zhang, F., Chen, S., Han, F., Lin, G., Zhai, Y., He, H., Zhang, J. and Ma, G. (2020). Associations between hydration state and pregnancy complications, maternal-infant outcomes: protocol of a prospective observational cohort study. BMC Pregnancy and Childbirth, [online] 20(1). doi:https://doi.org/10.1186/s12884-020-2765-x.
- Ciciu, E., Paṣatu‑Cornea, A.-M., Petcu, L. and Tuţă, L.-A. (2021). Early diagnosis and management of maternal ureterohydronephrosis during pregnancy. Experimental and Therapeutic Medicine, [online] 23(1). doi:https://doi.org/10.3892/etm.2021.10949.
- Harvard Health. (2013). Fight fatigue with fluids – Harvard Health. [online] Available at: https://www.health.harvard.edu/healthbeat/fight-fatigue-with-fluids#:~:text=When%20you%20are%20low%20on,help%20you%20maintain%20your%20energy.
- Diringer, M. (2017). Neurologic manifestations of major electrolyte abnormalities. Handbook of Clinical Neurology, [online] pp.705–713. doi:https://doi.org/10.1016/b978-0-444-63599-0.00038-7.
- Shaheen, N.A., Alqahtani, A.A., Assiri, H., Alkhodair, R. and Hussein, M.A. (2018). Public knowledge of dehydration and fluid intake practices: variation by participants’ characteristics. BMC Public Health, [online] 18(1). doi:https://doi.org/10.1186/s12889-018-6252-5.
- Negro, A., Delaruelle, Z., Ivanova, T.A., Khan, S., Ornello, R., Raffaelli, B., Terrin, A., Reuter, U. and Mitsikostas, D.D. (2017). Headache and pregnancy: a systematic review. The Journal of Headache and Pain, [online] 18(1). doi:https://doi.org/10.1186/s10194-017-0816-0.
- Ülker, K. and Çiçek, M. (2013). Effect of Maternal Hydration on the Amniotic Fluid Volume During Maternal Rest in the Left Lateral Decubitus Position. Journal of Ultrasound in Medicine, [online] 32(6), pp.955–961. doi:https://doi.org/10.7863/ultra.32.6.955.
- Alaa Farghal, M., Mohamed Zakaria, A.E.-M. and Abd El-Hamed Sedek, A.E.-M. (2021). ACUTE ORAL HYDRATION IN MANAGEMENT OF OLIGOHYDRAMNIOS AND DOPPLER CHANGES. Al-Azhar Medical Journal, [online] 50(1), pp.311–324. doi:https://doi.org/10.21608/amj.2021.139724.
- Figueroa, L., McClure, E.M., Swanson, J., Nathan, R., Garces, A.L., Moore, J.L., Krebs, N.F., Hambidge, K.M., Bauserman, M., Lokangaka, A., Tshefu, A., Mirza, W., Saleem, S., Naqvi, F., Carlo, W.A., Chomba, E., Liechty, E.A., Esamai, F., Swanson, D. and Bose, C.L. (2020). Oligohydramnios: a prospective study of fetal, neonatal and maternal outcomes in low-middle income countries. Reproductive Health, [online] 17(1). doi:https://doi.org/10.1186/s12978-020-0854-y.
- Alman, B.L., Coffman, E., Siega-Riz, A.M. and Luben, T.J. (2017). Associations between Maternal Water Consumption and Birth Defects in the National Birth Defects Prevention Study (2000-2005). Birth Defects Research, [online] 109(3), pp.193–202. doi:https://doi.org/10.1002/bdra.23569.
- Mulyani, E.Y., Hardinsyah, Briawan, D., Santoso, B.I. and Jus’at, I. (2021). Effect of dehydration during pregnancy on birth weight and length in West Jakarta. Journal of Nutritional Science, [online] 10. doi:https://doi.org/10.1017/jns.2021.59.
- Zhou, Y., Zhu, X., Qin, Y., Li, Y., Zhang, M., Liu, W., Huang, H. and Xu, Y. (2019). Association between total water intake and dietary intake of pregnant and breastfeeding women in China: a cross-sectional survey. BMC Pregnancy and Childbirth, [online] 19(1). doi:https://doi.org/10.1186/s12884-019-2301-z.
- Priya Soma-Pillay, Nelson-Piercy, C., Heli Tolppanen and Alexandre Mebazaa (2016). Physiological changes in pregnancy. Cardiovascular Journal of Africa, [online] 27(2), pp.89–94. doi:https://doi.org/10.5830/cvja-2016-021.
- Pruimboom, L. and Reheis, D. (2016). Intermittent drinking, oxytocin and human health. [online] ResearchGate. Available at: https://www.researchgate.net/publication/301745556_Intermittent_drinking_oxytocin_and_human_health



